
What is Plantar Fasciitis
Plantar Fasciitis is one of the most common causes of heel pain and can be a very debilitating condition. It typically causes a stabbing pain in the bottom of your foot near the heel. The pain is usually worse in the morning, making your first few steps very painful, although it can also be triggered by long periods of standing or when you get up from sitting.
What is the Plantar Fascia
The plantar fascia is a band of tissue, called fascia, that connects your heel bone to the base of your toes. It supports the arch of the foot and absorbs shock when walking.
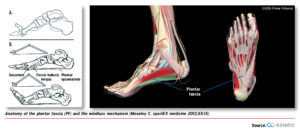
What Causes Plantar Fasciitis
Whilst the exact cause of the condition remains unclear and poorly understood, it appears that in some people, repeated load can cause this band of tissue to become irritated or possibly inflamed, causing pain.
Even though plantar fasciitis can develop without an obvious cause, some factors can increase your risk of developing this condition. They include:
Age. Plantar fasciitis is most common in people between the ages of 40 and 60.
Certain types of exercise. Activities that place a lot of stress on your heel and attached tissue — such as long-distance running, ballet dancing and aerobic dance — can contribute to the onset of plantar fasciitis.
Foot mechanics. Flat feet, a high arch or even an atypical pattern of walking can affect the way weight is distributed when you’re standing and can put added stress on the plantar fascia.
Obesity. Excess pounds put extra stress on your plantar fascia.
Occupations that keep you on your feet. Factory workers, teachers and others who spend most of their work hours walking or standing on hard surfaces can be at increased risk of plantar fasciitis.
Now the important bit!
What can I do about it?
PHYSICAL THERAPY
Exercises to help stretch the plantar fascia, achilles tendon, calf muscles have been found to be beneficial, but we have found that one of the most useful approaches is to start an exercise program to progressively load the plantar fascia. This specific exercise protocol has been shown to achieve better outcomes than stretching alone.
A guide to this type of loading can be found by following the link below, but please consult a medical professional first for advice and diagnosis before starting.
ICE
ORTHOTICS
Inner soles that prevent pronation have been reported to be beneficial in some cases
SELF MASSAGE
Some patients benefit from self massage with a tennis ball or rolling pin for example and sometimes can incorporate this into their ‘ICE’ treatment by using a bottle of frozen water and rolling their foot over that.
Surgical or other procedures
If more-conservative measures aren’t working after several months, your health care professional might recommend:
Injections. Injecting steroid medicine into the tender area can provide temporary pain relief. Multiple shots aren’t recommended because they can weaken your plantar fascia and possibly cause it to rupture. Platelet-rich plasma obtained from your own blood can be injected into the tender area to promote tissue healing. Ultrasound imaging during injections can assist in precise needle placement.
Extracorporeal shock wave therapy. Sound waves are directed at the area of heel pain to stimulate healing. This is for chronic plantar fasciitis that hasn’t responded to more-conservative treatments. Some studies show promising results, though this therapy hasn’t been shown to be consistently effective.
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.


